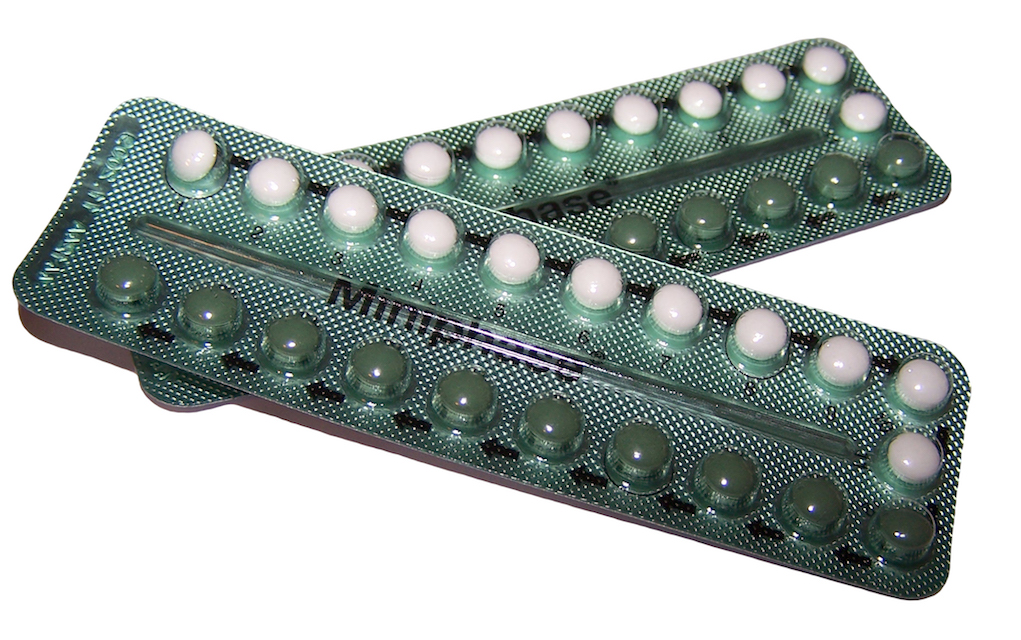
By 2015, the use of the hormone-based contraceptive pill or device has become almost as ubiquitous as vaccination or cheeseburgers. Touting many social benefits such as the emancipation of women from the risks of unplanned pregnancy, the contraceptive pill has become the mascot of modern feminism. Hormonal birth control allowed women to choose when they became pregnant and when not to and women were given the power to effectively liberate themselves from this sometimes oppressive relationship with nature.
With the growing popularity of Malthusian concepts of overpopulation and economic catastrophe during the 1960’s, the pill was seen as a biological saviour. It was proselytised across the globe as promoting smaller families and averting the imminent disaster of a population crash as humanity bred beyond the capacity of its resource base. This was particularly true in the poorer nations that struggled to feed and supply the basic needs of their people. Economic benefits also arrived with women entering the workforce in unprecedented numbers. The hormonal contraceptive pill was marketed in almost messianic terms by its developers and supporting politicians. A view welcomed by pharmaceutical companies that were set to make trillions over the ensuing decades.
Populations were already dropping steadily before hormonal contraception
Needless to say, women took to the new technology in their droves and were encouraged by doctors and often parents and partners concerned about preventing unwanted pregnancies. The benefits of the mass medicating of women’s reproductive cycles began to impact almost immediately with fertility rates declining in correlation with its expanded use. Though it is difficult to prove causatively, most reproductive and demographic specialists agree that hormonal contraception has certainly contributed to the reduction in the number of unwanted pregnancies and has also facilitated and favoured the general downsizing of family size norms. However, it is important to note that that fertility rates had been declining in most industrialised countries well before the pill existed. The parallel reduction in both mortality and fertility, usually called the demographic transition, began in many countries at the start of the 20th century and to some extent during the last part of the 19th century. This was well before modern contraceptives appeared.
The mean number of children broadly dropped from about six per woman to three or less during his time, even when birth control was not available. During this period, sterilisation was limited to strong medical indications and abortion was prohibited (although abortions were often performed illegally in bad conditions). This highlights that a substantial decline in fertility can occur for reasons other than the availability of efficient means of birth control. So this population decline in more developed nations shows that people were already finding highly effective ways of preventing unwanted pregnancies. Which begs the question, why did people flock to the use of the hormone driven pill if they already had effective means at their disposal?
In the past, having one or two children in the first years of marriage was quite natural, and subsequently the couple would usually investigate other means to prevent further pregnancies. This reveals a key feature of modern contraceptives, being that they are not significantly more effective (traditional methods could be used quite effectively by motivated couples) but that they are under the sole control of women and no longer linked to intercourse. A woman using the pill or an IUD is in a permanently infertile state until she stops using the method. If at any time she wishes to conceive, she has to decide to end this situation.
Therefore, she (or the couple) has to find good reasons for stopping her sterile state and start planning for pregnancy. Pregnancy began to become a somewhat predictive event that was planned in advance and guided by the contingencies of career and economics rather than a natural force to be deflected or succumbed to. Adding to this, it appeared that there were other medical benefits. Some women with fibromyalgia, endometriosis and other similar ailments were recommended the pill and it seemed that the pill was almost all pro’s with very few con’s. Of course over the next 40-years the health and associated “social costs” would begin to present themselves. The lack of rigorous studies and complete statistical data ensured that these were clarified only in hindsight.
From an economic perspective, the pill made possible the large-scale entry of women into the full-time job market and tertiary education. Beginning in the 1970’s this functioned as a powerful incentive for both ‘the market’ and policy makers to make contraception affordable and easily accessible. So the pill altered not only culture and the way we looked at reproduction but by delaying pregnancy it also promoted huge shifts in working demographics, and greater participation of women in society.
Signs of the pills sometimes dangerous side effects came in the late 1970’s and 80’s and saw some governments temporarily withdraw support for high-dose contraceptives. Recombined and low dose options in the 90’s and particular in the last decade saw that statistical risk lowered and side effects lessened. This allowed mass government subsidisation of the contraceptive pill to continue across the world making the pill a norm of most developed world couples and many single women’s lives. Meanwhile, ever more anecdotal information about the risks and consequences of hormonal control of reproduction was stifled by the lack of long-term, longitudinal and large sample studies of the ‘Pill’.
Risks for women, but not men?
Contradictions exist in the feminist argument for hormonal contraception liberating women. Yes, it did allow women to take control of their own reproductive cycles and fertility, but it also allowed the cascade of side effects which studies consistently demonstrated over the last 4 decades. Though it protects against much less common endometrial cancer it raises the risk of breast cancer which is the most common form of cancer for women and one of the deadliest. While it seems to lower the risk of ovarian cancer it raises the risk of cardiovascular disease and strokes which are the biggest source of pathological mortality for both men and women today. The list of side effects for the pill is deeply disturbing when you consider that 150 million women use it worldwide and that most do not understand the degree of risk they are taking.
- Increased risk of heart attack and stroke
- Migraines
- Higher blood pressure
- Gall bladder disease
- Infertility
- Benign liver tumours
- Decreased bone density
- Yeast overgrowth and infection
- Increased risk of blood clotting
- Lowered libido ( 15% long term to permanent even post pill )
- Increased risk of cervical and breast cancers
- Weight gain or loss
Something which is all the more disturbing is when you consider the reality of statistical collation via reporting. Often its only users and private doctors seeing side effects and contraindications. This can create a significant statistical under-representation of the health costs of using hormonal contraception. Worse still is that the reality of most of the studies done with large sample sizes, which are vital in order to get applicable population representation, were done in the 1960’s over 3-years only.
We do not currently have reliable and tested data on how the contraceptive pill affects cancer rates and other known contraindications such as thrombosis, strokes and cardiovascular disease over longer periods. Nor do we know how these potentially higher risks are even further magnified by obesity, chronic stress and the use of other medications like SSRI’s etc over more than decade-long time scales. Factors which were never considered in the majority of large-scale testing, but are major demographic variables in today’s world. So the true long-term impact on women’s health via the pill is still a very nebulous and poorly understood area.
We might consider this an enormous double standard by both governmental and medical authorities and society in general when actively promoting the use of hormones in young people. We have been very reluctant to allow young men to forever be plagued by the risks and consequences of early hormonal intervention. An easy example is steroid use, with its sale being largely illegal in most countries and there has been very little research into male contraception by comparison to female contraception. But society has been content to actively promote hormonal therapies along with their significant risks to our tens of millions of our teenage daughters. Hardly a humane or fair or feminist, stance to take.
So is the male hormonal pill an answer to the risks that women take?
Not likely. The business case for male hormonal contraception is unlikely to be scooped up by large pharmaceutical firms in the near future. As new discoveries are made and move into testing phase they are carefully trialled under strict medical oversight in a process lasting up to 10-years. Only when it is determined that no serious adverse effects are detected is it potentially released. Marketing plans are then initiated and business models devised to recoup investments. As opposed to statins or developing an obesity drug which could be used by a far larger portion of the population male hormonal contraception could only ever be used by a maximum of half the population.
Austrian-American scientist Carl Djerassi, dubbed the father of the female pill, said in a 2014 interview:
“This [resistance] has nothing to do with science; we know exactly how to develop [the male pill], but there’s not a single pharmaceutical company who will touch it – for economic and socio-political, rather than scientific, reasons.’ he said. “Their focus is on diseases of a geriatric population: diabetes obesity, cardiovascular, Alzheimer’s. Male contraception is nothing compared with an anti-obesity drug.”

Plus there is precious little evidence that the majority of men actually want to take over control over their reproductive ability. Even the most optimistic survey’s show that little over half would be even willing to try it. This hardly reinforces a business case for big Pharmaceutical companies to invest in such projects. Its seems, reflected in several surveys over the last decade, that men are quite satisfied with most of their options. Vasectomies (which in some cases are now reversible) have been a staple by men in the western world for years now. Condoms are cheap, simple to use and easily accessible. Condoms also have the added benefit of protecting the man against many STD’s.
Finally, at the risk of some serious twitter flack, it’s only fair to observe the likelihood that feminism and its marketing of the pill as a flagship for women’s liberation is somewhat averse to that same mass-adoption of the male pill. Since 1974 at the World Health conference in Budapest, where the first public discussions of a male pill were raised, feminist groups have insisted that reproduction should remain in the hand’s of women. Recently the feminist site ‘Jezebel’ called the male pill ‘whore pills’ while other articles including the ‘Guardians’ Angela Phillips piece warned that women would lose control of when they decided to get pregnant if the male pill was adopted widely.
This seems another one of those double standards prone to littering this topic like social and ethical land mines. Men may find that retaking the reproductive ground is more trouble than its worth, with female populations having grown entitled to choosing when those ‘happy accidents’ are to occur as well as when not. Considering the increasing knowledge of the impact of the pill on many women’s health, men in the more savvy internet era may be reluctant to risk their future health onto the altar of pharmaceutical profit and fallibility.
So for now, it seems its back to shared responsibility and the traditionally more mechanical approaches to contraception. It is worth raising the point that if the blind dedication of the last 40 years to hormonal contraception laden with relatively easy profit had not been the way – who knows how much further along, IUD and other non-hormone based technologies might have advanced. Certainly, the recent ‘Vasalgel’ non-hormonal approach to male contraception is an indication that at least now, non-hormonal methods are beginning to be explored for both men and women. This is certainly a step in a more equitable, potentially safer and more diverse direction for those seeking to decide when they wish to have children and when to not.